Understanding the male ejaculation anatomy and why your post-vasectomy test matters more than you think
Where does sperm actually live?
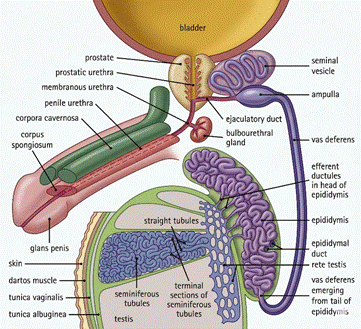
Most people assume sperm just sits in the testicles waiting to go. Not quite. Your testicles make sperm, but once produced, sperm moves into a tightly coiled tube called the epididymis — a structure so compact that if you unravelled it, it would stretch about 6 metres long. That’s where sperm matures and is stored, ready for action.
But here’s the thing most men don’t know: sperm doesn’t just sit there until you ejaculate. Between ejaculations, your body is quietly and continuously moving sperm along the vas deferens (the tube that gets cut during a vasectomy) toward a wider section near the prostate called the ampulla. Think of the ampulla as a staging area — a small holding bay where sperm waits just before the main event.
So what actually happens during ejaculation?
It’s a surprisingly complex, well-coordinated sequence — not just one big release.
As you become aroused, the vas deferens — normally a winding, curvy tube — actually straightens out and pulls taut, a bit like pulling a garden hose straight. The sharp angle between the ampulla and the seminal vesicle disappears, opening up a direct pathway for sperm to rush from the epididymis into the ampulla.
Just before ejaculation, the ampulla dumps its sperm-rich contents directly into the urethra via the ejaculatory duct. Importantly, sperm goes straight through — it doesn’t mix into the seminal vesicles first. That’s a common misconception.
The seminal vesicles (two small glands that produce most of the fluid in semen) then squeeze out about 10% of their contents per contraction. The prostate adds its own fluid too. All of this mixes together, pressure builds, and then — the first expulsive jet.
|
⚡ Fun fact Ejaculation isn’t one single squirt. The
seminal vesicles contract again and again, building pressure each time. On
average, there are around eight separate pulses per ejaculation. The
first couple carry the most sperm; the later ones are mostly fluid. Think of
it like a pump-action water gun — each pump builds pressure, then releases a
burst. |

And after it’s all over? The system doesn’t fully empty. Some of the mixed fluid that was sitting in the ejaculatory duct actually flows backwards into the ampulla — a bit like sauce settling back in the bottle when you put it back upright.
Things you’ve probably wondered
Why does your penis pulse during orgasm?
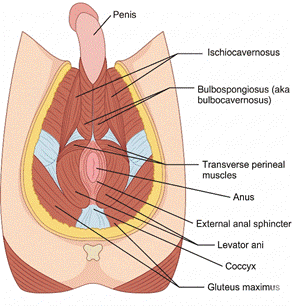
That pulsating sensation during orgasm isn’t random — it’s a muscle called the bulbospongiosus rhythmically contracting at the base of your penis. Each contraction squeezes the urethra and drives a burst of semen forward. Those contractions are the eight expulsive jets we just described — you’re feeling the engine that powers the whole process. It’s a reflex you can’t consciously control during orgasm, but it’s the same muscle you can train with pelvic floor (Kegel) exercises.
Why do some men ejaculate more forcefully than others?
Same reason some people can throw a ball harder — muscle strength. The force of ejaculation depends on pelvic floor muscle tone, how much pressure has built up before the first release, and how aroused you were beforehand. Younger men tend to ejaculate more forcefully because pelvic floor tone naturally declines with age. Men who do regular pelvic floor exercises often notice a real difference — it’s a trainable skill, not a fixed trait.
What if very little comes out – or nothing at all?
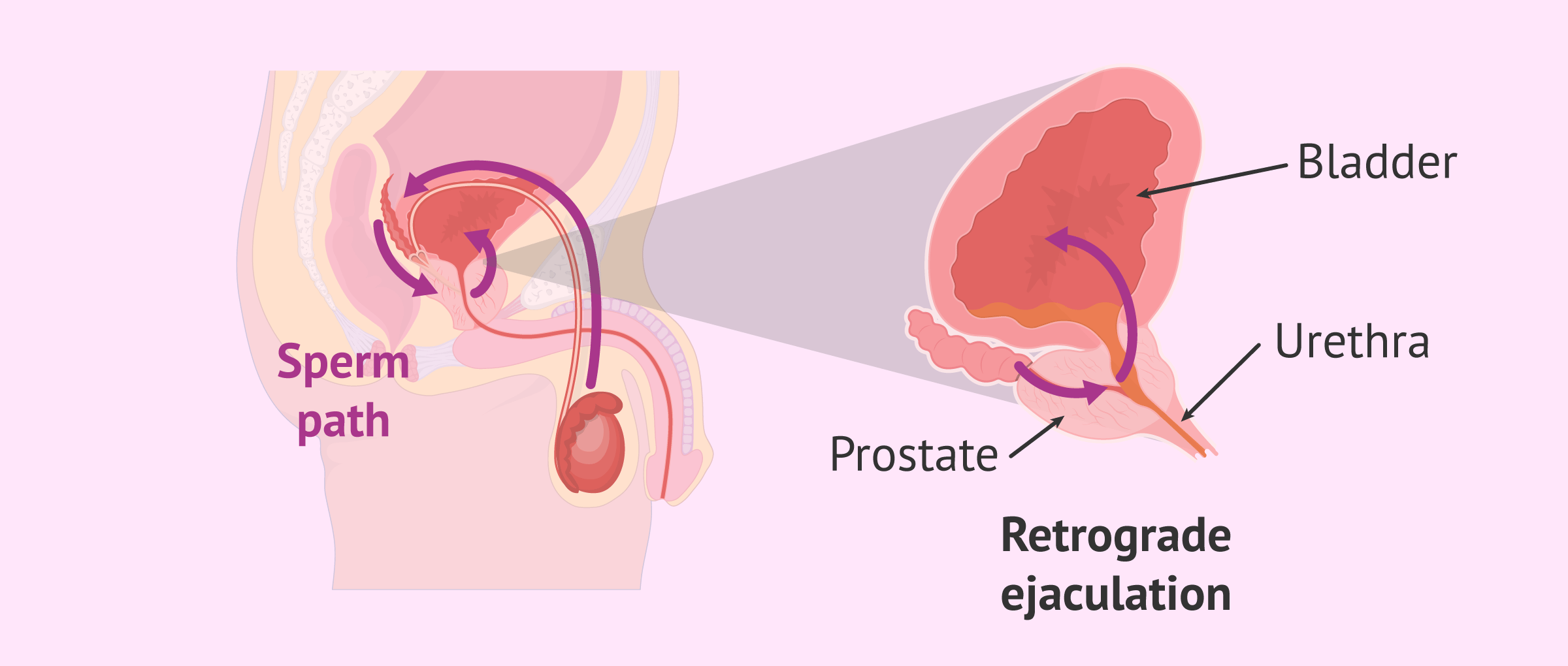
Some men notice that they orgasm but produce very little or no semen. This is called retrograde ejaculation — instead of being propelled forward through the penile urethra, semen travels backwards into the bladder. It happens because a small muscular valve at the neck of the bladder (called the internal urethral sphincter) that normally snaps shut during ejaculation doesn't close properly. The orgasm still feels normal — you just don't see much come out. Common causes include prostate surgery (especially TURP), diabetes that has affected the nerves controlling the bladder neck, and certain medications such as Tamsulosin (Flomax) and some antidepressants. It's harmless, but if you've had a vasectomy and experience this, it's important to let your doctor know before your post-vasectomy semen test — a low-volume sample may not accurately reflect whether you've cleared your residual sperm, and a urine sample after ejaculation may need to be checked as well.
What if ejaculation feels weak or dribbles rather than pulses?
If ejaculation has always been low-force, that's likely just your baseline pelvic floor tone — and pelvic floor exercises can help. But if it's changed over time, or if you also notice a weak or split urinary stream, it could be a sign of a urethral stricture — a narrowing of the urethra caused by scar tissue. Think of it like a kink in a hose: the same pressure is being generated behind it, but the flow is restricted. Common causes include previous urinary infections, catheterisation, or procedures involving the urethra. A stricture doesn't affect your fertility or vasectomy clearance, but it can make ejaculation feel less satisfying and may affect how your semen sample is produced. If you've noticed a gradual change in the force of your ejaculation or your urinary stream, it's worth mentioning to your GP.
Why do some men produce more semen than others?
Semen volume varies hugely — anywhere from about half a millilitre to 11 mL, roughly the difference between a teaspoon and a tablespoon. About two-thirds of the fluid comes from the seminal vesicles, with the prostate contributing most of the rest. Sperm itself makes up less than 5% of the total volume.
How much you produce depends on the size of these glands, your hydration, how long it’s been since you last ejaculated, duration of arousal, and your testosterone levels. Volume tends to peak after about 5–7 days of abstinence, then plateaus.
|
⚡ Fun fact Since the vas deferens contributes almost
nothing to semen volume, a vasectomy makes no noticeable difference to
how much you produce. The fluid looks and feels the same — it just no longer
contains sperm. |
Does more semen actually feel better?
There’s some logic to it — more fluid means more sustained stretch of the urethra during ejaculation, and potentially more contractions needed to expel it, which could make orgasm feel longer. Some men do notice that ejaculations after a few days’ abstinence feel more satisfying.
But the honest answer is that orgasm intensity is mostly about your brain, not your volume. Arousal, anticipation, how connected you feel with your partner, and your overall health all matter more than millilitres. If you want better orgasms, pelvic floor exercises, adequate foreplay, and cardiovascular fitness will get you further than any supplement.
Why does any of this matter after a vasectomy?
When you have a vasectomy, the vas deferens is cut and sealed partway along its length — well away from the ampulla and the seminal vesicles. Everything “downstream” of the cut is completely unaffected. You still ejaculate normally — the fluid just no longer contains sperm, once the existing sperm have cleared out.
And that’s the key point: at the time of your vasectomy, there are already sperm sitting in the ampulla. They need to be flushed out through subsequent ejaculations before you can be considered clear.
Why can’t I just ejaculate 20 times and call it done?
Because the ampulla isn’t the same in every man. The inside can look very different from one person to another. In some men, it’s smooth-walled and tubular — sperm passes through easily and clears out quickly. In others, the inner lining is covered in folds, pockets, and crevices. In these men, sperm can get temporarily trapped, only to be flushed out gradually over many ejaculations.
|
⚡ Fun fact In one study, the man with the most residual
sperm after vasectomy had 4,745 times more sperm remaining than the
man with the least. And you can’t predict who’s who from a pre-vasectomy
sperm count. It’s purely about the internal architecture of the ampulla,
which varies naturally between individuals. |
On top of that, remember the “backflow”? After each ejaculation, some fluid settles back into the ampulla. And between ejaculations, your body keeps moving small amounts of sperm along the vas toward the ampulla by natural muscle contractions. So the ampulla keeps getting small top-ups for a while.
This is why a fixed number of ejaculations doesn’t work reliably. Some men clear in 4 ejaculations. Others still have sperm at ejaculation 10 or beyond. The only way to know for sure is to test.
Why do we wait about 3 months?
Two reasons. First, it gives enough time for the vast majority of men (over 90%) to have cleared their residual sperm. Testing too early — say at 4 weeks — and only about a third to half of men will be clear, even though the vasectomy is perfectly fine. That leads to unnecessary worry and repeat testing.
Second, the 3-month mark is a good window for picking up the rare event of early recanalisation — where the cut ends of the vas rejoin themselves. Most early recanalisations happen within the first 3 months, so testing at this point serves double duty: confirming clearance and screening for early failure.
What if my test still shows a few sperm?
Don’t panic. If a small number of non-moving (dead) sperm are found at your post-vasectomy test, this is usually completely normal and doesn’t mean your vasectomy has failed. Remember those ampullary folds and pockets? In some men, a handful of dead sperm can trickle out for months.
Guidelines allow what’s called “special clearance” if the count is very low (under 100,000 non-motile sperm per mL). This is well-established practice and doesn’t require a repeat procedure.
What would raise concern is if motile (swimming) sperm are found at 3 months or later, or if your count goes back up after being zero. That pattern suggests recanalisation rather than simple residual clearance, and would need further investigation.
|
The short version Your body is
remarkably well-engineered for getting sperm from A to B. After a vasectomy,
it takes time for the leftover sperm in the downstream plumbing to clear —
and how long that takes depends mainly on the unique internal shape of a
structure most men have never heard of. That’s why the post-vasectomy semen
test isn’t optional — it’s the only way to confirm you’re actually clear. Three months. One test. Peace of mind. |



